Are Payers Ready to Comply with the 21st Century Cures Act?
What health plans need to meet the ONC interoperability rule.
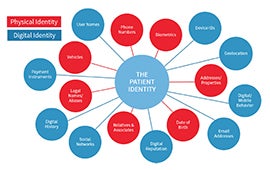
As part of the 21st Century Cures Act, the interoperability rule seeks to drive patient access to their own personal and medical data and supports the ability to share that data, allowing patients more power to coordinate their own healthcare.
The new rule bolsters the existing trend toward a more patient-focused model, which will empower patients to participate more effectively in their own medical care and improve public health services.
Payer organizations will need to able to gather and share data around patient costs and coverage, clinical interactions, and other data points. All of these efforts aim to prevent information blocking and improve the flow of easy patient access to or transfer of data.
 Payers have been working toward achieving interoperability going back to the 2003 implementation of HIPAA’s version 4010 electronic transaction standards guidance. More broadly across healthcare, the first stage of Meaningful Use has also encouraged the sharing of electronic health information across health care providers.
Payers have been working toward achieving interoperability going back to the 2003 implementation of HIPAA’s version 4010 electronic transaction standards guidance. More broadly across healthcare, the first stage of Meaningful Use has also encouraged the sharing of electronic health information across health care providers.
However, as deadlines for the 21st Century Cures Act are starting to be reached, most payer organizations are not fully prepared to comply with the new interoperability rule. This is due in part to the complexity and lack of clarity surrounding the new requirements.
• What sort of identity authentication must be required to allow access?
• How long do payers have to send the data once a request has been made?
These questions and more have created inevitable delays in reaching compliance with the new rule. Additional challenges exist around adhering to new Fast Healthcare Interoperability Resources (FHIR) standards, conforming to new public reporting mandates, and of course developing the root capacity to ingest and communicate out patient health information and other data from multiple sources while maintaining patient privacy and data security.
As access to and transfer of protected health information (PHI) becomes common, it will only increase the need to ensure that appropriate authentication and security measures are in place. All of these new functions will require substantial funding and potentially new third-party partnerships to meet these stringent IT needs.
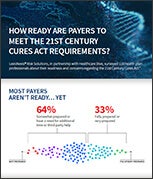
 Understandably, payers have concerns as they progress toward full compliance. In partnership with Healthcare Dive, we surveyed 110 health plan professionals about their readiness and concerns regarding the 21st Century Cures Act. 38% of respondents are primarily focused on the need to protect patient privacy and adhere to security standards. Regardless of the top concern, survey participants indicated that the most helpful capability they need to be successful is clean, high-quality data.
Understandably, payers have concerns as they progress toward full compliance. In partnership with Healthcare Dive, we surveyed 110 health plan professionals about their readiness and concerns regarding the 21st Century Cures Act. 38% of respondents are primarily focused on the need to protect patient privacy and adhere to security standards. Regardless of the top concern, survey participants indicated that the most helpful capability they need to be successful is clean, high-quality data.
As payers plan for the future, they should look beyond current system data and consider use cases that may become possible with enriched data sets. Evaluate new potential data integration capabilities and how they may improve payers’ ability to support data security and privacy beyond the current requirements. Forward-thinking organizations may find that by developing their own capabilities outside the scope of the 21st Century Cures Act, they open up new opportunities to benefit patients as well their own organizations.
Meeting the new interoperability requirements is not a simple task, but the tools and expertise are available to help your organization succeed. At LexisNexis Risk Solutions Health Care, our high-quality data and analytics are helping healthcare stakeholders to meet the new data requirements and lead the way toward patient-centered care and better outcomes. Download the infographic and study to learn more about what payers are saying about their readiness for the new interoperability requirements.
Video: Data Sharing Opportunities Healthcare Has Never Seen Before
Access Full Infographic
Access Full Study
Meet Interoperability Requirements

Products You May Be Interested In
-
Instant Verify for Healthcare
Accelerate identity verifications with a solution customized to fit your workflow
Learn More -
InstantID® for Healthcare
Identify fraud risks across exchanges and broker communities
Learn More -
InstantID® Q&A for Healthcare
Seamlessly verifies the identity of patients, medical staff and pharmacists.
Learn More -
Keep Contact
Transform your engagement efforts by improving and maintaining patient and member data.
Learn More -
Multi-Factor Authentication for Healthcare
Authenticate members and providers
Learn More