Creating healthier communities starts with clear, connected insights into individuals and populations
Better Understand Your Population with Critical Social Risk Data and Insights

Solutions that Deliver Results for Public Health Agencies


Identity Assessment & Assurance


Fraud Detection & Prevention


Data Quality Management
Vital Records Management
Meaningful Impact in Public Health

Success in Finding Contact Details
Using LexisNexis® Accurint® for Government, two metro-Atlanta counties increased their ability to locate individuals with STDs.
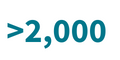
Contact Tracers Trained
LexisNexis Risk Solutions supported more than 20 states in training contact tracers during the COVID-19 pandemic.

Agencies Use Our Solutions
We work with a vast majority of U.S. Federal, state and local government agencies.
Insights and Resources
Products You May Be Interested In
-
Gravitas®
Unlock the power of real-world data for healthcare with a comprehensive data network and next-generation de-identification technology.
Learn More -
EssentialID™
Ensure fast and secure access to government programs with LexisNexis EssentialID™. Our seamless identity proofing process provides unparalleled global insights, speed, security, and transparency.
Learn More -
LexID® and SALT for Government
Gain a more complete view of individuals and businesses in your agency by linking together records.
Learn More -
Accurint® for Government
Locate and identify people, businesses and assets
Learn More -
AmplifyID™
AmplifyID leverages decades of identity intelligence expertise and insight to preserve program integrity, provide equitable access and prevent fraud across Federal, state and local government.
Learn More -
AmplifyID™ Master Person Index
Ensure equitable access and smooth service delivery with a precise, whole-person view
Learn More -
Multi-Factor Authentication for Healthcare
Authenticate members and providers
Learn More -
VitalIQ™
Simplify and automate vital records management and transactions with VitalIQ™ .
Learn More



